Telangiectasia
Self Help Group
FACT
SHEET 1.
Introduction
Hereditary
haemorrhagic telangiectasia (HHT) also known as Osler-Weber-Rendu disease, was
first described over 100 years ago. It is due to a faulty gene and is very
variable causing some people considerable distress while others escape with
much less severe problems. For the majority of patients, nosebleeds are the
main problem although bleeding from the lining of the stomach and the
intestines occurs in about 20% of cases.
How do I know if I have HHT?
HHT
does not usually cause any problems in early life. The first sign that a child
has HHT is usually nosebleeds that are heavier and more frequent than those of
other children. Over half of all patients with HHT have frequent nosebleeds by
the age of 16 and over 90% by the age of 30 years. The other feature of HHT is
the red spot or telangiectasia. These spots are actually tiny malformed blood
vessels, which are found particularly on the lips, tongue and fingertips. If
you are over 30 and do not have nosebleeds or any little red spots
(Telangiectases) on your hands or lips then it is unlikely that you have HHT.
Very
occasionally the faulty gene may be inherited and that person may not show any
signs of HHT. Usually however, if you do not have any signs of HHT by the age
of 30, it means you have inherited the good copy of the gene and so do not have
a faulty copy to pass on to your children.
What is the risk of me passing HHT on to my children?
In
order to answer this question we have to go through some basic genetic facts.
Everything about us from eye colour to blood groups is coded for by units of
inheritance or GENES. We each have over 50,000 pairs of genes, one of
each pair from our mother and one from our father. Each time we make an egg or
sperm, we put one member of the pair in. The process is random, like tossing a
coin.
The
diagram below shows what can happen when a parent with HHT has a child:
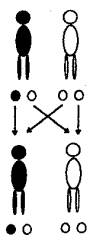
Affected Parent Other parent
One HHT gene and one normal gene Two normal genes
One gene passed on from each parent
Affected child Unaffected child
HHT gene from affected parent
and normal gene from other parent Normal genes from both parents
You can see from the diagram that 50% of the time,
the affected parent passes on the faulty copy of the gene. If this happens then
the child will develop HHT. Each child of a person with HHT has a 50% risk of
developing HHT. It does not depend on the sex of the child or whether or not
previous children are affected. If you have 4 children in a row that develop
HHT then the risk to the 5th child is still 50%.
I have been diagnosed as suffering from HHT. What tests
should I have?
If you have regular heavy bleeds from your nose or
stomach and intestines, your doctor will monitor your blood to see if you
become anaemic. This enables prompt treatment with iron tablets or a blood
transfusion where necessary.
About
20% of patients with HHT have a problem with blood vessels in the lungs. This
is called Pulmonary Arterio-Venous Malformation ( PAVM ) and can cause problems
if it is not treated. We recommend that anyone with HHT is checked out for this
problem. PAVMs can be detected on X-ray and by measurement of oxygen levels in
the blood using an oximeter. It is particularly important to be screened if you
have a relative with a PAVM.
Other
rare complications of HHT may need specific investigations. Your doctor will
advise you if they are necessary in your case.
What
treatment is available?
The
best person to advise you about the treatment you require is your General
practitioner or Hospital specialist. However, the following is a brief guide:
Anaemia
Any
patient that has regular episodes of bleeding is at risk of becoming anaemic.
Anaemia is a medical term used when there is insufficient iron in the blood.
Iron can be replaced in 2 ways; either by taking iron tablets or by a blood
transfusion. Where possible your doctor will attempt to keep your blood iron
levels up with iron tablets. Occasionally, if you have a very severe bleed then
you may need a blood transfusion.
Nosebleeds
Various
treatments have had some success in some patients but as yet there is no “magic
cure”.
Cautery
of
troublesome vessels can produce temporary relief but long-term results are not
so good. Most ENT surgeons tend to use cautery very sparingly as repeated
cauterisation may lead to damage of the surrounding nasal lining.
Oestrogens ( hormone treatment ) can
be effective, particularly in women but may lead to troublesome side effects in
male patients which limit usefulness.
Laser
treatment Like
cautery this treatment is aimed at a specific bleeding site. If you have
several telangiectases in the nose or intestines then laser treatment is less
effective but the results of treatment in patients with small numbers of spots
are quite encouraging. However the equipment involved is very expensive and
treatment is only available at specialist centres.
Skin
Grafts
Nasal skin grafts are a “last resort” treatment when there is uncontrollable
severe bleeding. The results are very variable.
PAVM
The
majority of PAVMs can now be treated radiologically. A fine tube is passed
through a vessel in the top of the arm or leg and small Teflon coated balloons
or steel coils are introduced through it to block off the abnormal vessels.
Blocking off these vessels should reduce the risk of complications from PAVMs.
Again treatment is available only at a few specialist centres. In this country,
the team at the Hammersmith Hospital have most experience of the technique.
Bleeding into the stomach and intestines
If
you have problems with bleeding into the stomach and intestines, your doctor is
likely to refer you to a gastroenterologist for an endoscopy. This test
involves looking at the upper portion of the gastro-intestinal tract with a
fibre-optic tube ( Endoscope ) the end of which is swallowed. If there are one
or two particular bleeding sites these can be treated by laser, frequently to
good effect. However there are often several sites of bleeding and in this case
your doctor may elect to try some form of hormone treatment or to treat you
“symptomatically”, that is with iron and blood transfusions.
SUMMARY
1
The
symptoms of HHT are variable. Although HHT can be a major problem for some
patients, others have infrequent nosebleeds or a few red spots.
2
It
is important to look for treatment complications such as PAVM and all patients
should have at least one chest X-ray and an estimate of arterial oxygen
saturation.
Mary Porteous
Consultant Clinical
Geneticist
Western General Hospital
Trust
Crewe Road
Edinburgh EH4 2XU
Tel: 0131-651-1012 FAX: 0131-651-1013
This Pamphlet was prepared
and written by Dr. Mary Porteous on behalf of the
Telangiectasia Self Help
Group, 39 Sunny Croft, Downley, High Wycombe, Bucks, HP13 5UQ
Tel: 01494 528047
www.telangiectasia.co.uk